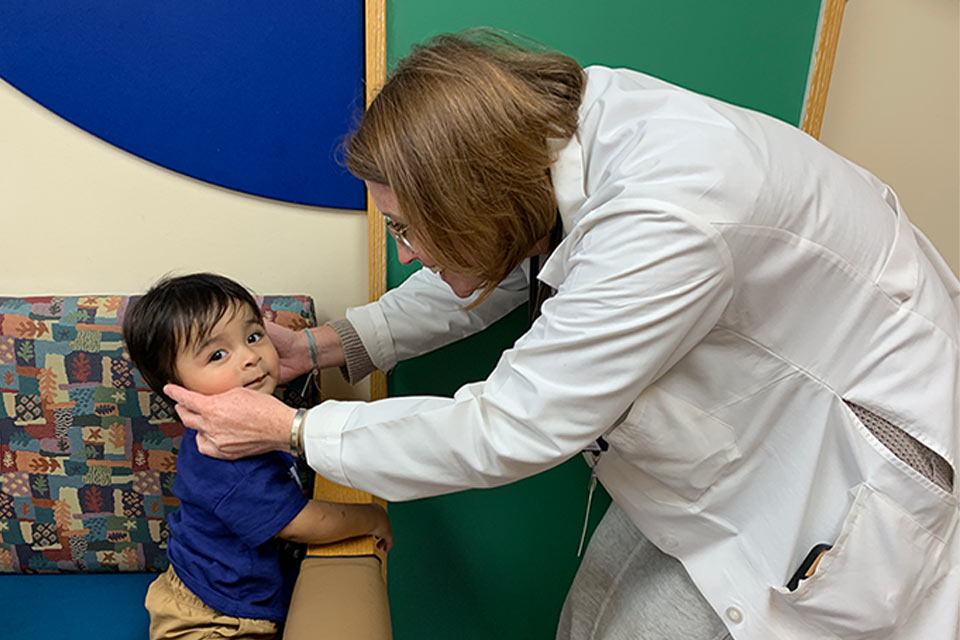
Sean :
Nous étions excités de savoir ce que nous allions avoir pour notre deuxième enfant. Et le médecin a rapidement identifié qu’elle allait être une fille. Puis, il a continué à prendre des mesures, et quelques minutes plus tard, il est sorti en disant : «Je pense que je remarque quelque chose ici.» C’était, tout d’abord, qu’il lui manquait un os au bas de la jambe. Il a également remarqué que l’os supérieur de sa cuisse était courbé et pas aussi long que la jambe droite.
Dr Robert H. Cho :
Dans le cas de Gianna, elle avait une jambe essentiellement non fonctionnelle sous le genou. Même si elle avait pu faire certaines choses avec cette jambe non fonctionnelle, elle n’aurait pas été capable d’en faire autant que si elle avait été amputée et appareillée avec une prothèse. Ce genre de décision n’est pas prise à la légère, mais nous avons la chance de nous occuper d’autant d’enfants atteints de cette maladie.
Devon :
C’était très effrayant, très inattendu. Vous y allez pour connaître le sexe de votre bébé, et vous découvrez qu’il y a d’autres problèmes à régler. Il l’a appelé déficience focale fibulaire proximale.
Sean :
Heureusement, le mari de notre gynécologue-obstétricienne était orthopédiste. Et il était ami avec le médecin-chef de l’Hôpital Shriners à Los Angeles. Très rapidement, nous avons pu parler au téléphone avec lui et un orthopédiste, et ils nous ont expliqué de quoi il s’agissait et à quel type de vie nous pouvions nous attendre. Ils ont aussi parlé des procédures d’allongement de la jambe et des amputations. Nous espérions certainement une procédure d’allongement de la jambe, mais à mesure que cet écart augmentait, nous avons commencé à réaliser que cette option n’était probablement pas aussi viable pour elle.
Devon :
Elle est née et elle était parfaite. C’était un moment si calme et paisible… Comme nous avions déjà Sofia, et qu’elle avait une grande sœur… Je me suis dit «Allons-y».
Elle avait environ trois mois. Nous avons eu notre première visite dans une clinique des Hôpitaux Shriners. La beauté de tout ça, c’est que nous avons pu voir un autre enfant qui avait peut-être un an, ainsi qu’un autre de trois ans, et même des enfants de cinq, sept et neuf ans. Nous avons donc vu ces autres enfants qui étaient là, et qui souriaient, et qui riaient, et qui étaient là avec leurs familles. Et j’ai pu visualiser ce que mon enfant allait être, et comment elle allait être. C’est pourquoi nous avons choisi les Hôpitaux Shriners. Nous savions qu’il ne s’agissait pas seulement d’une opération chirurgicale et que nous serions ensuite laissés à nous-mêmes. Nous avions une communauté. Il y avait des physiothérapeutes, il y avait des gens pour nous aider avec des services dans notre communauté. Des médecins, des processus. C’était une communauté de personnes et de familles, et nous savions que c’était l’endroit où nous pourrions l’accompagner à long terme.
Le jour de l’opération, nous sommes allés à l’hôpital. Nous sommes arrivés très tôt le matin, c’était une journée calme. Même si Gianna ne s’en souvient probablement pas, je suis sûr qu’il y a eu beaucoup de traumatismes. C’est un traumatisme physique que vous faites subir à votre enfant. Et c’est quelque chose qui, en tant que parent, est très effrayant. Mais elle s’en est sortie comme une championne.
Gianna :
Je me souviens d’être arrivée à l’Hôpital Shriners, d’avoir franchi ces portes et de m’être sentie bien accueillie. Les gens là-bas étaient si patients avec moi, et tellement ouverts à essayer de me donner la meilleure
jambe possible. Je sais qu’en tant qu’enfant, j’ai été difficile dans certains cas. Mais ils ont toujours fait en sorte que je me sentais digne d’être là, et j’avais l’impression que je pouvais tout faire.
Conférencier 6 :
Bonne fille, Gigi.
Sofia :
TU AS RÉUSSI!
Devon :
Son prothésiste était Tony Ellis. Il la mettait à l’aise. La relation entre un prothésiste et un patient est tellement intime.
Anthony Ellis :
Elle a aujourd’hui la même personnalité qu’elle avait quand elle avait un an. Elle était très enjouée, très sociable. Elle n’hésitait pas à aller à la rencontre des étrangers qui entraient dans la pièce. Elle était ce genre de personne.
Devon :
La confiance et l’amour qu’ils ont construits ensemble. C’était vraiment un processus incroyable, sachant que lorsque nous sommes arrivés là-bas, il n’y avait aucune peur chez elle. Elle avait une routine, des gens qu’elle connaissait. Denis était incroyable. Il est également amputé, donc en tant que parent, il a pu me dire comment laver la prothèse. Des détails simples que je ne connaissais pas, qu’il pouvait partager avec nous pour nous faciliter un peu la vie.
Denis Jordan :
Gianna était très précoce. Elle était, je dois le dire, une enfant sauvage. Peu importe ce que quiconque considérait comme un handicap, elle n’en avait pas. Vous ne pourriez pas avoir de meilleur patient, pour être honnête avec vous. Intrépide, juste prête à foncer.
Devon :
Gianna repoussait toujours les limites, dépassant toujours jusqu’où elle pouvait grimper dans un arbre, à quelle vitesse elle pouvait aller. Elle se poussait toujours à suivre sa sœur, à suivre les enfants du quartier et à foncer, foncer, foncer, foncer, foncer.
Gianna :
Ma sœur faisait toujours du sport et elle était active dans notre communauté, alors je l’ai toujours admirée et j’ai toujours voulu être comme elle. Donc, je suis sortie et j’ai essayé le sport. J’ai joué au soccer, au softball, j’ai fait un peu d’escrime. J’ai fait du tennis quand j’étais plus jeune, j’ai fait de la natation. Quelle que soit l’activité qu’elle faisait, je voulais essayer aussi.
Sofia :
Je pense que nous avons un lien spécial, car je ne suis pas seulement comme une protectrice à cause de sa jambe, mais sa sœur aînée. Surtout maintenant, je pense que notre relation s’est beaucoup développée à mesure que nous vieillissions et devenons plus matures.
Matthew :
Ce qui me rend fier de Gianna, c’est qu’elle est capable de faire plusieurs activités à la fois, si elle le veut. Si elle veut faire quelque chose, elle se décide simplement. Au lieu de tergiverser à ce qui pourrait arriver. Elle fait juste ce qu’elle veut.
Corey Lerner :
Elle était notre meilleure joueuse en double. Et elle, en tant que personne dans son ensemble, m’inspire vraiment et elle inspire aussi les autres filles. Parce qu’elle arrive sur le terrain avec beaucoup de vigueur et d’énergie, et elle motive l’équipe non seulement en tant qu’individu, mais juste en mettant tout le monde dans l’ambiance du tennis.
Christina Rising :
Je pense que Gianna est une personne très réceptive aux commentaires, ce qui, à mon avis, est une très bonne chose pour une étudiante. Avoir la confiance nécessaire de pouvoir entendre les critiques et être capable de les accepter, d’en tirer des leçons et d’en grandir, c’est une démonstration de sa capacité et de sa confiance.
Devon :
Une chose que je savais quand Gianna est née, c’est qu’elle allait faire de nous de meilleures personnes. Elle allait faire de moi une meilleure mère, elle allait faire de moi une meilleure épouse, elle allait faire de moi une meilleure personne. Et je pense qu’elle a fait ça pour nous tous dans la famille. Elle relève la barre. Nous n’avons pas beaucoup d’excuses dans cette maison.
Sean :
Je pense que ce qui me rend le plus fier d’elle, c’est juste comment elle grandit, comment elle persévère. Comment elle se lève tous les jours et sort du lit, met sa jambe. Je dois comprendre qu’il n’y a pas de journée facile pour elle, mais elle a toujours la bonne attitude pour se lever et partir.
Gianna :
Quand je pense que mon père est un Shriner, je me sens tellement reconnaissant envers lui, ma famille, les Shriners et les maçons. Parce qu’il s’est intégré à cause de moi. Il a rejoint une communauté, et il en fait partie, et il change les choses aux Hôpitaux Shriners. Ce dont je suis la plus fière dans ma vie, c’est probablement ma personnalité et ma confiance. Parce que j’ai traversé des moments où je ne pensais pas que j’allais être la personne que je suis aujourd’hui. J’étais vraiment déprimée, j’étais vraiment au plus bas. Je ne croyais pas en moi. Je suis fière de qui je suis devenue. Quant à l’héritage que je laisse derrière moi, je veux être une personne vers laquelle les gens se tournent pour être encouragés et inspirés. Je veux être la personne qui fait preuve de force, de vulnérabilité et d’honnêteté. Je veux montrer aux enfants comme moi que les limites sont infinies et qu’ils peuvent faire ce qu’ils veulent. Vous devez être actif et vous devez essayer.
Juan Diego :
Je m’appelle Juan Diego. Bienvenue à Tegucigalpa, ma ville natale située au Honduras. C’est un endroit où je suis né et où j’ai grandi, comme n’importe quel enfant normal.
Jackie :
[Espagnol 00:11:40].
Juan Carlos :
Je me souviens qu’il était mon meilleur ami. J’ai toujours voulu jouer avec lui, dans mon équipe et tout. Et je le défendrai toujours. Oui, parce que je suis son frère aîné, et depuis tout petit, je suis très protecteur envers lui.
Juan Carlos :
[Espagnol 00:12:50].
Juan Diego :
Quand j’avais 13 ans, ma mère a décidé de déménager dans un nouvel appartement, qui était au troisième étage face à une rue en construction. Comme il était en construction, l’appartement n’était pas totalement terminé. Il y avait une fenêtre sans vitre donnant sur la rue, à la même hauteur que le lampadaire avec des fils à haute tension devant.
Jackie :
[Espagnol 00:13:29].
Juan Diego :
Plus rapidement qu’un clin d’œil, j’ai juste ressenti toute la charge, toute l’électricité traversant littéralement mon corps. C’est si rapide, vous n’avez pas le temps de réagir. Mon cœur s’est mis à battre très vite, au point que je sentais qu’il allait exploser. Et soudain, toutes les lumières se sont éteintes, et je me suis senti comme si j’étais dans cette grotte, tout seul. Parce que j’ai pu entendre ma mère crier d’inquiétude.
Jackie :
[Espagnol 00:15:02].
Juan Diego :
Tout à coup, je me suis réveillé vraiment effrayé. Parce qu’un des voisins me faisait des manœuvres de réanimation. Je voyais cinq personnes autour de moi qui me demandaient si ça allait. Elles m’ont donné de l’eau, et j’ai essayé de me lever, mais je n’ai pas pu. Évidemment on ne m’a pas laissé faire, mais je ne comprenais pas pourquoi je ne pouvais pas me lever. Je me sentais juste comme si je n’avais pas de bras, parce que je n’étais pas capable de le bouger. C’est là que j’ai réalisé, et j’ai regardé autour de moi, et j’ai vu mes mains brûlées.
Jackie :
[Espagnol 00:15:51].
Juan Carlos :
[Espagnol 00:15:54].
Juan Diego :
Jour après jour, je sais ce que signifie être un survivant de brûlures et de vivre tous les processus, toutes les douleurs. Je me souviens d’une nuit où j’ai commencé à ressentir ce sentiment d’impuissance. L’une des infirmières a appelé ma famille, et je me souviens d’environ 10 personnes qui essayaient de passer par cette petite porte, et qui essayaient juste de me dire «Salut, salut». Je me souviens d’avoir eu un sourire sur mon visage, mais des larmes dans mes
yeux, juste de les voir. J’ai commencé à constater à quel point ces personnes étaient spéciales, et j’ai commencé à sentir que je n’étais pas seul.
Jackie :
[Espagnol 00:17:45].
Juan Carlos :
[Espagnol 00:18:47].
Juan Diego :
Je me souviens être allé à mon premier rendez-vous. Ils étaient vraiment gentils et prudents avec moi, comme quand il a fallu enlever mes pansements. Ils comprenaient, parce qu’à l’époque, je n’avais pas vu mes mains. Mes parents venaient de me dire qu’on allait devoir m’amputer les doigts, mais je n’avais pas regardé.
Jackie :
[Espagnol 00:19:51].
Courtney Updegrove :
Je pense que la première chose que je dis toujours à propos de Juan Diego, c’est qu’il a la meilleure attitude que vous puissiez avoir. Il a un bel avenir devant lui. Il regarde toujours vers l’avant. Et je dis toujours qu’il est l’une de ces étoiles brillantes que tout le monde recherche toujours.
Dr Joseph Upton :
C’est assez extraordinaire. Parce que la brûlure est passée par un bras, puis par l’autre bras, et le cœur est entre les deux. Et généralement, ils ne survivent pas. Et lui, bien sûr, a survécu. Il fallait lui donner un ressenti, une sensation. Bien sûr, j’adore faire cela chez les enfants, car ils obtiennent d’excellents résultats. Cela consiste essentiellement à faire une greffe nerveuse : on prend des nerfs ailleurs dans son corps et on les déplace dans sa main.
Dr Branko Bojovic :
Je dirais qu’une partie de mon rôle dans ses soins consistait à prendre ce genre de forme et d’apparence, et à améliorer certaines des choses que nous examinerions du point de vue de l’apparence, et à complimenter les gains fonctionnels qu’il a déjà eus, et à aider afin d’adoucir le tout en termes de beaucoup de ses cicatrices. Juan Diego a une réputation, il est connu comme le maire de l’hôpital. Quand il se présente, c’est presque comme s’il y avait un cortège qui l’amenait.
Juan Diego :
C’était juste après ma chirurgie de greffe nerveuse, j’avais ces énormes cicatrices sur la main. Je me souviens avoir demandé à mon médecin : «Docteur, pensez-vous que je vais avoir une cicatrice?» Et il a répondu très sérieusement : «Nous sommes des chirurgiens. Nous ne laissons pas de cicatrices ici.» Je me disais que ce serait impossible. Cet homme est quelque chose. Comme il l’a dit, un mois plus tard, je ne voyais plus de cicatrice. Et à ce jour, vous ne voyez aucune cicatrice ici. C’est ainsi que je peux résumer le traitement aux Hôpitaux Shriners.
Juan Carlos :
Juan Diego, c’est comme une lumière dans la noirceur. Peu importe où il se trouve, il brille toujours. Il tire toujours le meilleur de chacun, et c’est pourquoi je pense que c’est un grand leader. Il y a cette phrase que nous disons maintenant dans notre famille, comme quoi les plus grandes batailles sont données aux plus grands guerriers de Dieu. Et bien, c’est la bataille qui a été donnée à Juan Diego.
Jackie :
[Espagnol 00:23:38].
Juan Carlos :
[Espagnol 00:23:38].
Juan Diego :
Techniquement, je ne suis pas censé être en vie. Je ne suis pas censé avoir de mains. Cela m’étonne. Le but de tout cela est de montrer à quel point Dieu est bon. Venir ici, c’est comme le plus grand retour auquel vous pouvez penser. Cinq ans après l’accident, revenir en aussi bon état que moi, avec cette attitude, en espérant aider tant de gens en tant que patient-ambassadeur international. C’est comme rire à la face de cet immeuble, parce qu’il ne pouvait tout simplement pas m’arrêter. Parce que ce n’était pas moi, c’était ma famille qui m’aidait, mes amis, et dans l’ensemble Dieu souverain. Ce n’est pas grâce à moi. C’est simplement grâce à toutes les personnes qui m’ont aidé, y compris les Shriners.